The worsening HIV crisis in Eastern Europe and Central Asia
- 31.05.2023 14:36
- Post Views: 528
Originally posted on Aidspan
According to the Global AIDS Update 2022, Eastern Europe and Central Asia (EECA) has the fastest growing HIV epidemic in the world. In 2021, 160,000 [130,000–180,000] people were newly infected with HIV — a 48% increase since 2010. There were 44,000 [36,000–53,000] AIDS-related deaths in the region in 2021, 32% higher than in 2010.
The UNAIDS report tells us that regional HIV prevention and treatment service coverage remains insufficient. As of 2021, 63% of people living with HIV (PLHIV) were aware of their status, 81% of people who knew their HIV-positive status were on treatment (51% of all PLHIV) and 94% of people on treatment were virally suppressed (48% of all those infected). Unsafe injecting practices are a key factor in the region’s epidemic. Opioid agonist therapy (OAT) is available in Armenia, Kazakhstan, Kyrgyzstan and the Republic of Moldova, but it barely reaches those in need in Kazakhstan and is unavailable in Turkmenistan and Uzbekistan.
The figure below indicates the dire state of the region’s epidemic.
Figure 1.Number of new HIV infections and AIDS-related deaths, EECA, 2000–2021
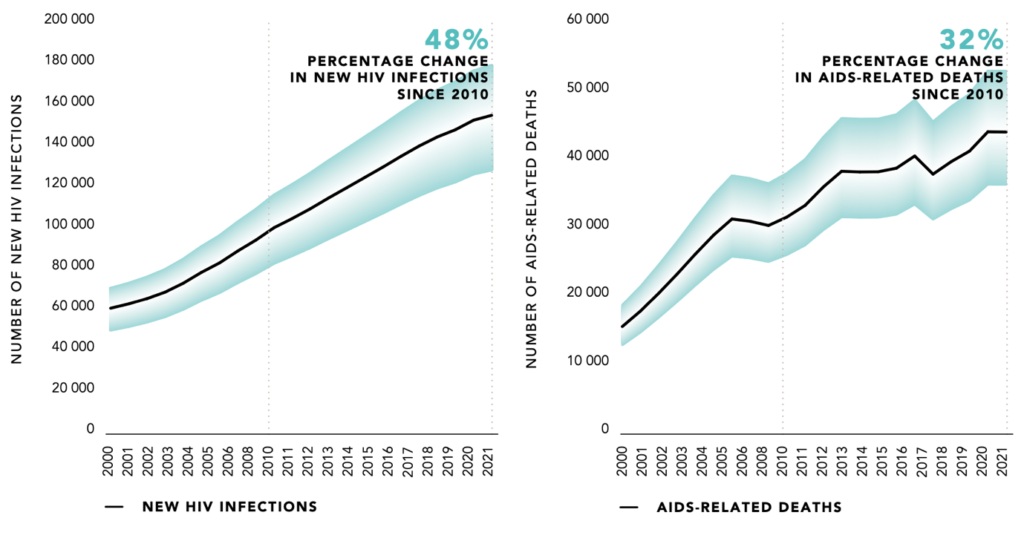
The next two figures shows how the epidemic is being driven by men who have sex with men (MSM) and people who inject drugs (PWID).
Figure 2. Distribution of acquisition of new HIV infections by population and sex (aged 15–49 years), EECA, 2021
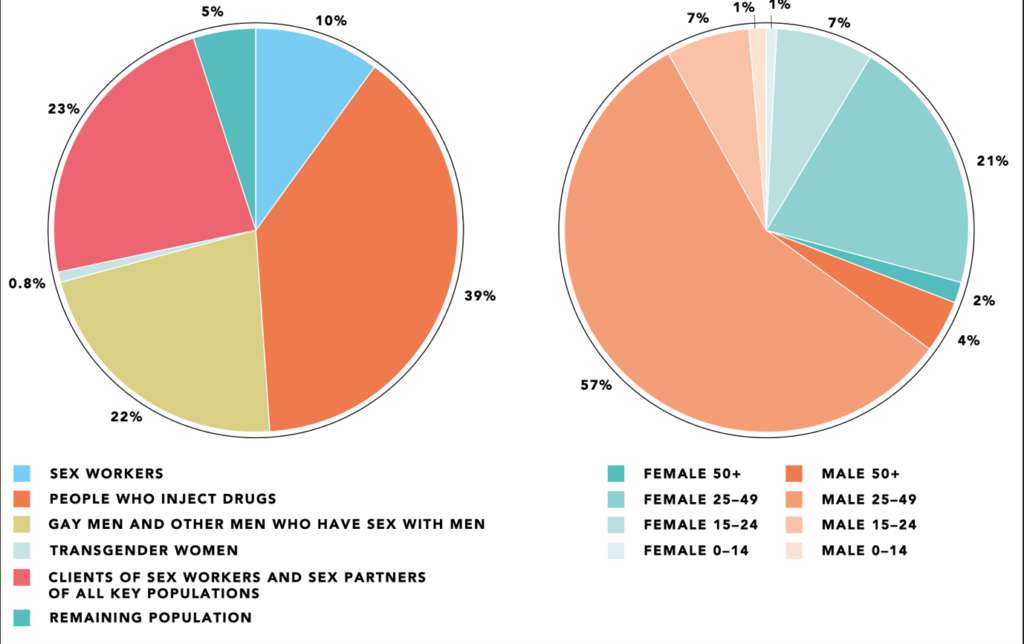
Source: Global AIDS Update 2022
Figure 3. HIV prevalence among key populations compared with adults (aged 15–49 years), reporting countries in EECA, 2017–2021
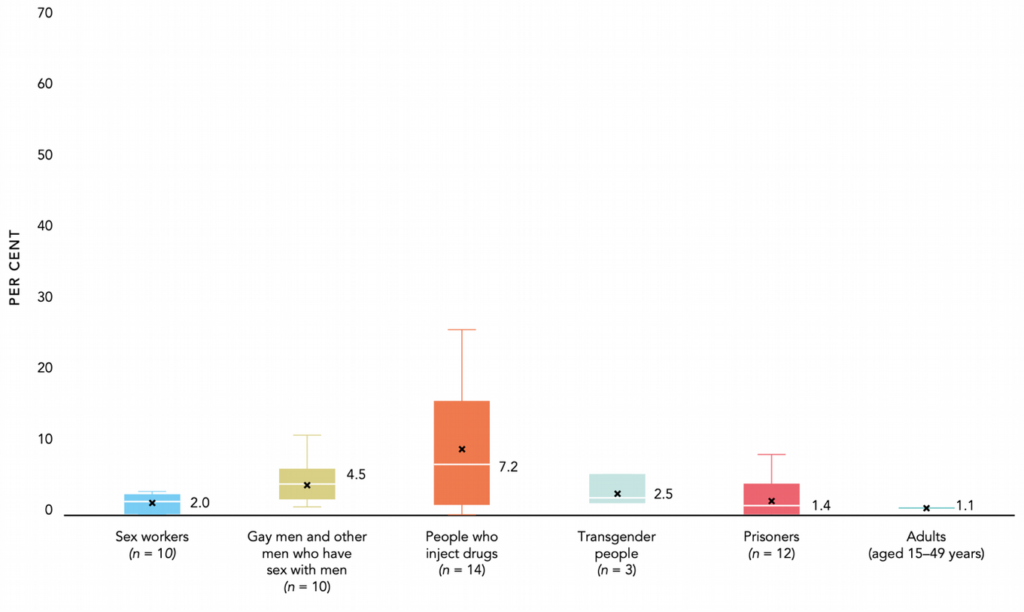
Source: Global AIDS Update 2022
Stigma and discrimination are a significant hindrance to effective HIV responses. Studies have documented high levels of stigma against HIV and key populations (KPs): in Tajikistan, for instance, only 23% of PLHIV surveyed reported a positive experience after disclosing their HIV-positive status. COVID-19 also highlighted an epidemic of violence against women across the region; and it increased women’s economic liabilities which in turn made them more vulnerable to sexually transmitted infections, including HIV, and unwanted pregnancy.
Legal and policy frameworks vary across the region. HIV transmission, exposure and non-disclosure are criminalized in all countries except Bosnia and Herzegovina and North Macedonia, although prosecution varies from country to country. Sex work and drug use are decriminalized in some countries in the region, but prosecutions still occur for organized sex work and possession of drugs. While some countries (Armenia, Kazakhstan, Kyrgyzstan, the Republic of Moldova and Tajikistan) have decriminalized same-sex sexual relations, stigma against gay men and other MSM remains common, including reports of police violence.
Russia’s invasion of Ukraine has fuelled the epidemic
One doesn’t usually think of this region as suffering from the population movements seen in other parts of the world that are subject to war and other upheavals. But in February 2022, the Russian Federation invaded Ukraine, home to 240,000 [220,000–280,000] PLHIV. The war has driven a humanitarian crisis, badly damaging health infrastructure in Ukraine and leading to widespread disruption of health services. Moldova, Poland and other countries in the region have also been affected by the large population movements of Ukrainians flooding across the borders. Maintaining access to health services (including the region’s largest OAT programme), as well as food, housing and personal safety, has proven especially challenging for the more than 15.7 million people requiring urgent humanitarian assistance and the more than 7.1 million displaced by the war, including PLHIV.
Resource for HIV prevention are almost non-existent
The population most affected by the rise in new infections are PWID and their families; high treatment costs and lack of funding for effective interventions increase their vulnerability.
Since 2018, data from 12 countries suggest that only 6% of HIV resources have been allocated to prevention. Most countries rely on domestic funding for prevention services for PWID , but some countries still depend on international resources for 100% of their programme. Current domestic spending on programmes is neither sufficient to meet necessary coverage for achieving the 2025 targets nor to reduce HIV incidence. Additional funding is required to alter the trajectory of new HIV infections.
According to UNAIDS, the economic impact of the ongoing war crisis in Ukraine on the EECA region appears to be significant, just as the global economy is showing signs of recovery from the COVID-19-induced crisis. In 2021, 88% of resources for HIV in the region were from domestic sources. The total resources for HIV in the region must grow 2.3-fold by 2025 to achieve the targets set out in the 2021 United Nations Political Declaration on HIV and AIDS: Ending Inequalities and Getting on Track to End AIDS by 2030.
Financial sustainability is now exceedingly unlikely
Sustainable government funding of HIV prevention programs has still not yet been achieved. Even countries such as Croatia, Montenegro, and North Macedonia, which were once presented as successful models of transition and sustainable HIV responses, are now facing challenges due to factors such as a lack of legal framework, political deprioritization of HIV, or frequent changes in government. Current resources are way below the estimated need, as shown in Figure 4.
Figure 4. Resource availability for HIV, EECA, 2006–2021, and estimated resource needs for HIV by 2025
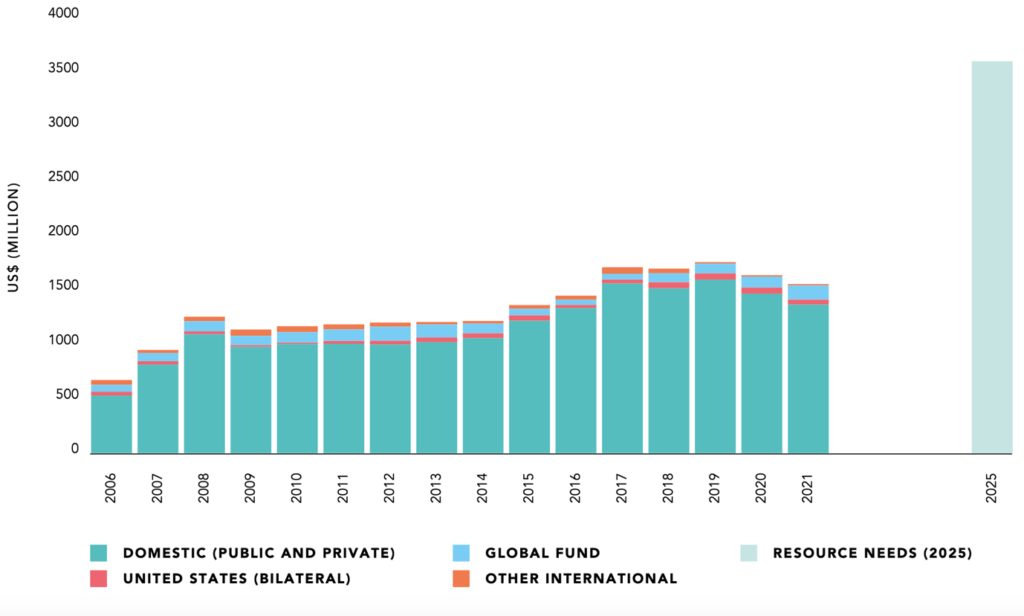
Source: Global AIDS Update 2022
The Global Fund has provided valuable regional advocacy programs that have been flexible in addressing new challenges. Community organizations have been able to adjust and respond to issues ranging from the war in Ukraine to the de-prioritization of HIV in North Macedonia and the eradication of HIV prevention programs in Bosnia and Herzegovina. However, sustained advocacy is essential in the face of these complex challenges and, for this, significant funding is required. The governments in the region and the Global Fund need to prioritize the funding of HIV prevention and treatment programs. However, lasting change and sustainable solutions can only be achieved through the advocacy and engagement of affected communities.
International organizations need to step up to the plate
Funding is also needed to address the social stigma associated with HIV/AIDS in EECA. This stigma often prevents PLHIV from accessing healthcare and support services. Advocacy campaigns are necessary to raise awareness about HIV/AIDS and reduce discrimination and stigma. Funding is required to support these campaigns and ensure they reach the most vulnerable communities. In addition to harm reduction programs and advocacy campaigns, funding is necessary for research into new HIV prevention and treatment strategies. Pre-exposure prophylaxis (PrEP) is an innovative approach to HIV prevention and treatment that offers hope for reducing the spread of HIV in EECA but much more needs to be done to increase knowledge about it in the region, and ensure that the most vulnerable groups can access it more readily.
The HIV response in the EECA region heavily relies on the active participation and leadership of civil society organizations (CSOs) and affected communities. It has been observed that some Global Fund partners have been facing challenges in terms of their commitment to advocating for sustainable HIV prevention and treatment programs in the region. The World Health Organization (WHO) country offices in the region have struggled to prioritize HIV prevention and treatment programs due to limited capacity and competing priorities at the country office level.
Additionally, UNAIDS has a limited presence in EECA, and its voice in advocating for a sustainable HIV response has been weak. This lack of support from international organizations has placed a heavy burden on CSOs and communities that are already facing significant challenges, including the recognition of some as foreign government agents in some countries.
In conclusion, there is a clear need for continued funding for sustainability and advocacy on HIV in EECA. Governments, international organizations, and donors must prioritize funding for HIV prevention and treatment programs, harm reduction programs, advocacy campaigns, and research to address the HIV epidemic in EECA. Affected communities, organizations, and civil society groups must be given a voice in the decision-making process. Efforts must also be made to reduce the stigma and discrimination faced by PLHIV. By investing in these critical areas, we can work towards a future where HIV/AIDS is no longer a threat to the lives and well-being of people in the region.
Services for migrants and refugees from Ukraine – HIV/TB care with a focus on key populations
Due to the increasing flows of refugees from Ukraine because of Russia’s invasion of Ukraine, the EECA Regional Platform created a spreadsheet to fill contacts details of face-to-face and online services for refugees and migrants (with a focus on HIV/TB care and key population groups).
Regional Platform – EECA
This web-resource is a part of new regional communication and coordination project “Regional Civil Society and Community Support, Coordination and Communication Platform - EECA”, implemented by Eurasian Harm Reduction Association (EHRA).
Tags
See also
-
EECA’s Regional Platform monthly Newsletter #24, May 2026 25.05.2026 11:05
-
EECA’s Regional Platform monthly Newsletter #23, April 2026 17.04.2026 15:54







